Avascular necrosis (AVN) is a death of bone tissue caused by lack of blood supply. The disease is also popular by other names like osteonecrosis, aseptic necrosis or ischemic necrosis.
Bone is a living tissue. It looks like a honeycomb from inside. Osteoblasts are the cells which grow into bone. Mature bone tissue is made up of osteocytes. When the osteocytes don’t get enough oxygen and nutrients they die. This is similar to heart attack wherein part of heart muscle dies when it does not receive oxygen and nutrients. AVN in that sense is a ‘bone attack.’ It can lead to breaks in the bone. It starts from a small area in the bone and eventually more and more part of bone dies. Smooth shape of bone deteriorates. Affected bone no longer fits into its desired position and the entire joint gets disturbed. This is called bone collapse. It is an extremely painful condition so much so that the patient cannot move that particular joint.
The most affected age group is between 20-40 years of age. Also, it is more common in men than women with an observed male to female ratio of 5:1.
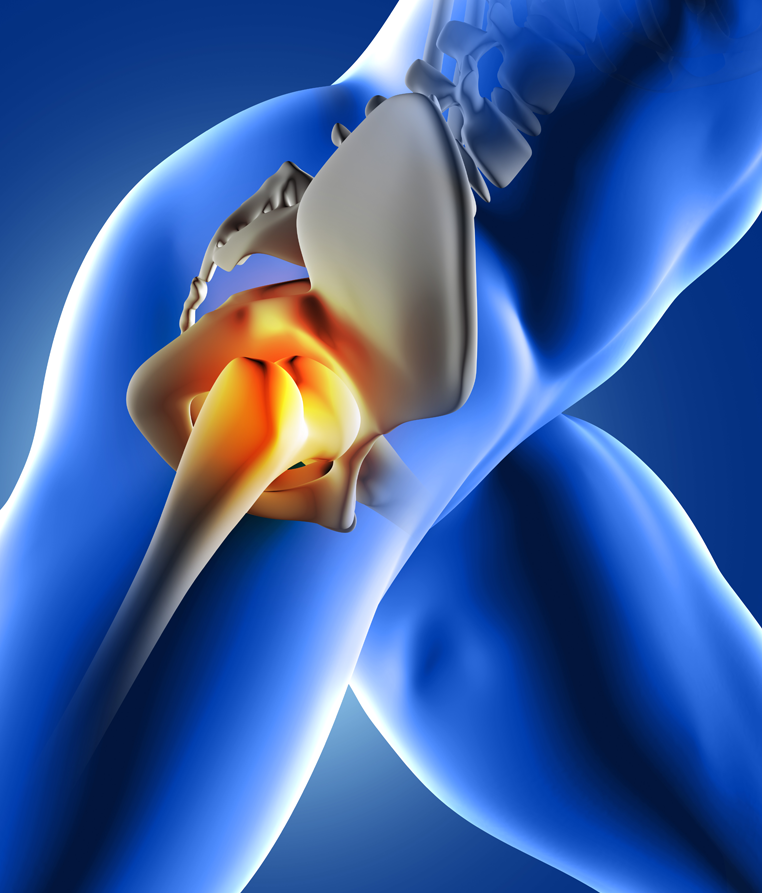
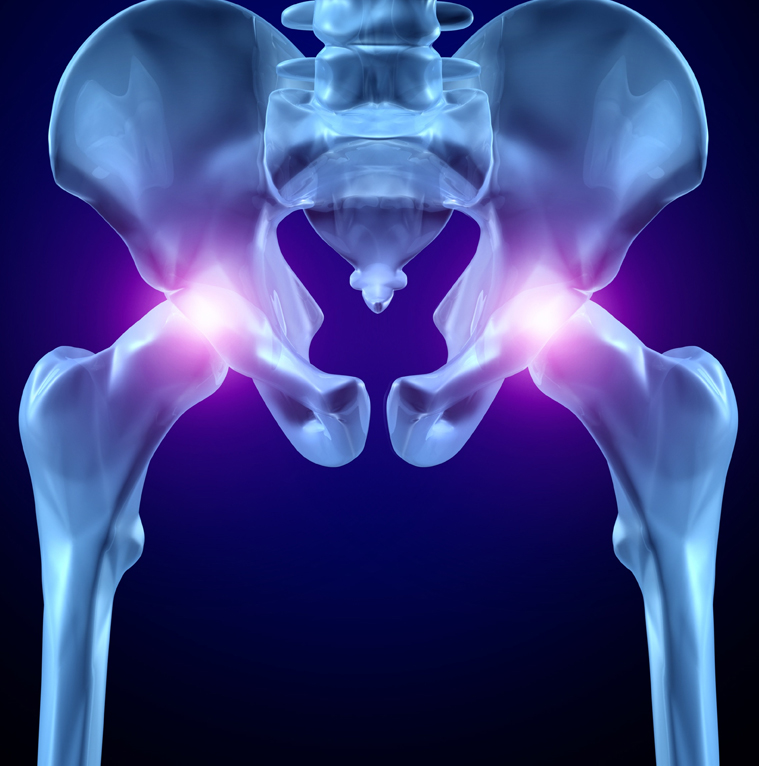
AVN can occur in all major joints of your body, most commonly in the Hip.
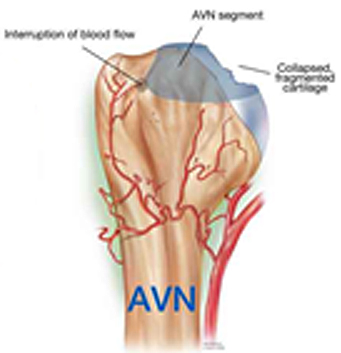
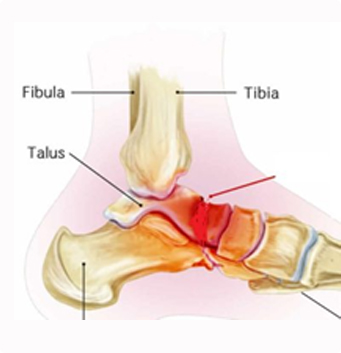
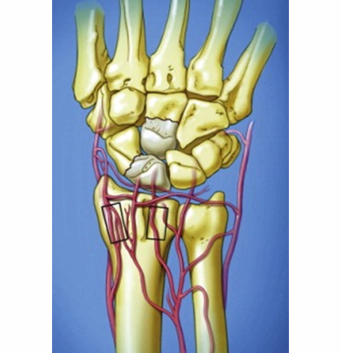
The hip joint is a ball and socket joint. It connects the thigh bone (femur) to the hip bone. The thigh bone is the longest and strongest bone in the body. It supports all of the body’s weight in activities like walking and running. When blood supply to the head of the thigh bone is temporarily cut off or permanently reduced, the bone begins to die. As the disease progresses, the round head of the bone flattens and appears as a deflated football. Due to this deformation, structure of the entire joint is disturbed leading to collapse.
In more than 60% of the cases, both the hips are involved. This condition is called bilateral AVN. When AVN is diagnosed in one hip, the other hip is also checked to rule out the possibility of bilateral AVN.
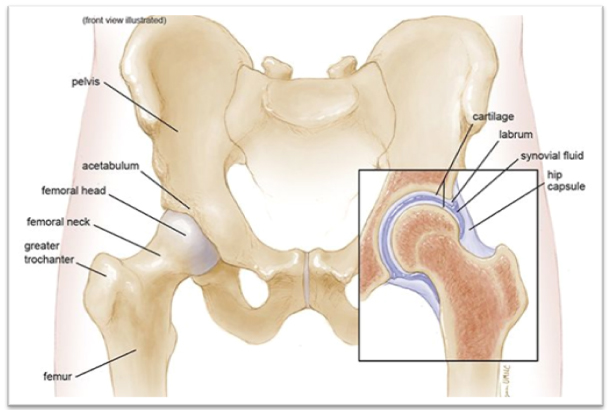
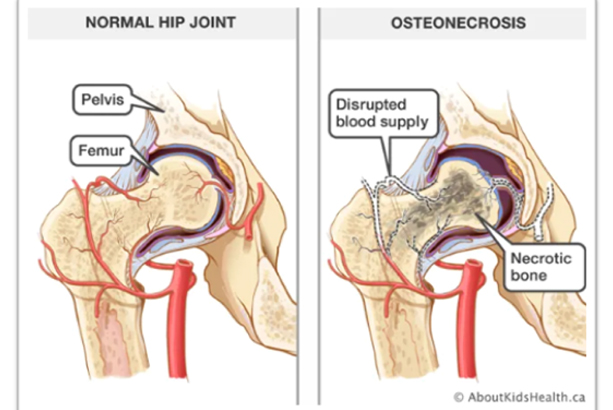
of femoral head
AVN could be caused due to trauma or some other reasons (non-traumatic). In most instances defining the cause of AVN is difficult. But the common causes include intake of steroids, heavy alcohol intake. It could be also due to some disorders like lupus, rheumatoid arthritis or sickle cell anemia. Though the mechanism may vary, end result is the same, i.e. interruption in the blood supply to the bone. There are cases where the cause is not identified despite in-depth investigation. Such cases are called idiopathic. In almost 40% of the cases, cause of AVN is unknown.
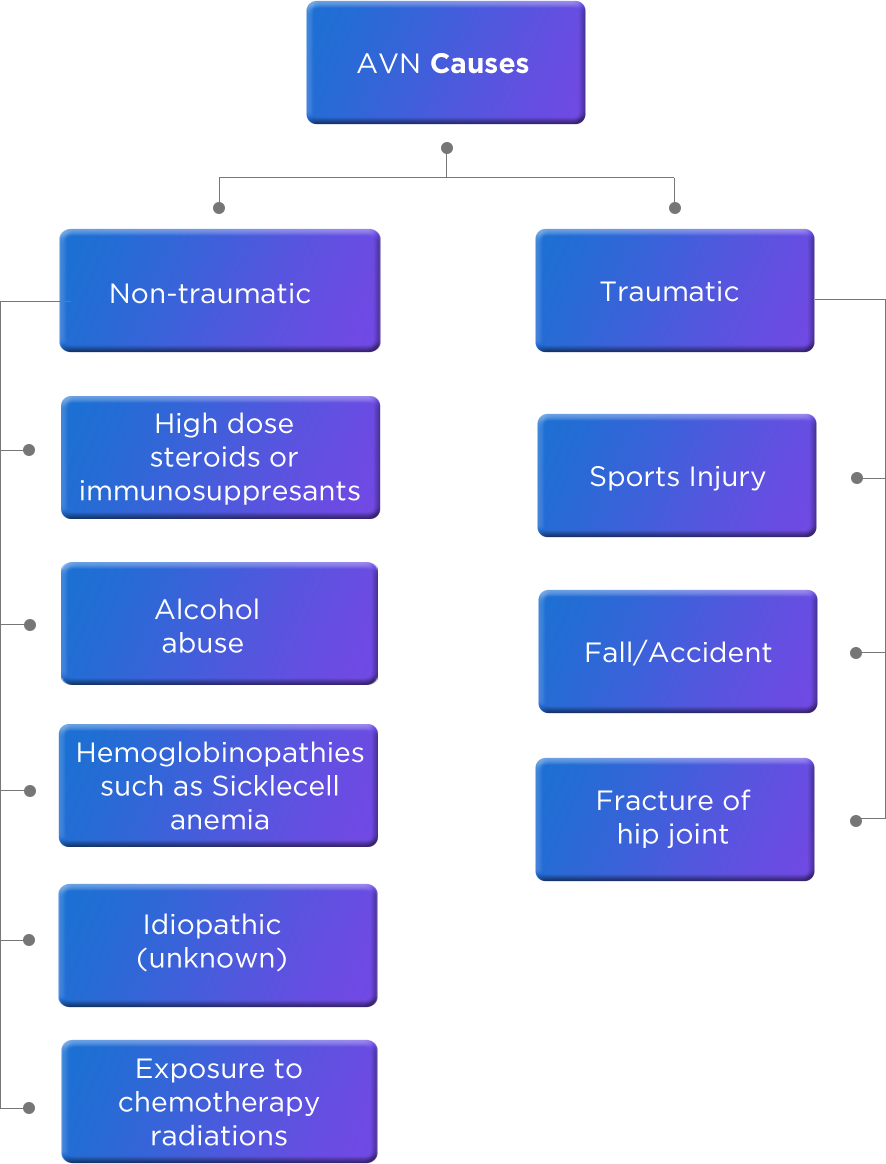

steroids or
immunosuppresants
abuse
such as Sicklecell
anemia
(unknown)
chemotherapy
radiations
As high as 35-40% cases of AVN are due to use of high doses of corticosteroids.5 Corticosteroids are medicines commonly used for suppression of immune system. Under diseased condition or injury body produces immune response. This is called inflammation. Pain, redness, swelling and increase in temperature are signs of inflammation. Anti-inflammatory medicines are required to manage these signs of inflammation. In addition to specific disease treatment, these anti-inflammatory medicines play important role in the treatment as they relieve the patient from troublesome symptoms including pain. Corticosteroids are thus routinely used in variety of skin and eye infections, in treatment of cancer, in solid organ transplant surgeries and even COVID 19 infections. Research says that exposure to high dose of corticosteroids in such situations for extended period significantly increases risk of AVN (as high as by 20-fold4).
Asthma is one condition which affects millions of people globally. Severe asthma is treated with corticosteroids, particularly when other treatments fail to control the disease. A study conducted by GlaxoSmithKline in 2016 has reported effects of corticosteroid exposure in severe asthma patients. Patients with severe asthma who received corticosteroids for longer duration had higher risk of developing AVN6.
Daily alcohol consumption or consumption in higher amounts (more than 4 drinks on any day or more than 14 drinks per week) for prolonged duration (8-20 years) increases the risk of alcohol induced AVN. Alcohol as a cause of AVN is seen in almost 20-40% cases5
Direct injury to the bone such as fracture of the femoral neck or dislocation of hip disturbs blood vessels in the bone. Due to this disturbance terminal branches of blood vessels which supply blood to the head of femur bone get damaged. The head of femur bone does not get blood. Whether traumatic or non-traumatic, AVN is due to interruption of blood supply. It could be due to break or block in the blood vessel or due to compression of the blood vessel.
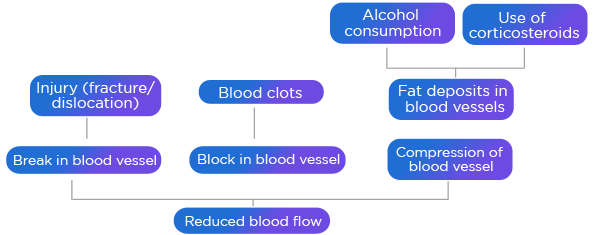
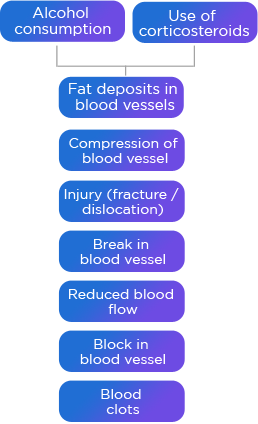
When the bone cells die, new cells are formed naturally to repair the damage. These new cells form a network in dead porous bone. However, it cannot attain the structure like the healthy bone. As a result the bone breaks. When the bone breaks the joint does not remain intact and it collapses.4
Avascular necrosis of the femoral head is a degenerative condition. Many people have no symptoms in early stages of the disease. As the disease progresses from mild to severe stage, symptoms increase gradually. Most common symptoms include-
- Hip pain and Hip rotation difficulty
- Pain in buttock area
- Groin (area between abdomen and upper thigh) pain radiating to the knee
- Intense pain at rest and during movement
- Limited movements of the joint
- Loss of mobility
- Limping

In the US, AVN is diagnosed at a rate of 1,20,000 to 1,60,000 new cases per year. Prevalence of bilateral disease, i.e. the disease affecting both the hips, is also high. According to a Japanese survey, 2500 − 3300 cases of AVN of hip occur each year.
In India, there is rise in incidence of AVN. This could be correlated to increase in steroid use and increase in alcohol consumption, which are the two major risk factors.
AVN of femoral head is one of the major indications for total hip replacement. According the report of Indian Society of Hip and Knee Surgeons Registry in 2019; as high as 50% of the total hip replacements are diagnosed to be due to AVN. There has been a rapid rise in joint replacement surgeries in India in past two decades. An Indian survey had reported occurrence of almost 70,000 joint replacement surgeries in the year 2011. This was predicted to increase at a rate of 26.7% during 2010-2017 to reach a figure of approximately 1 lakh. In India, AVN cases are projected to reach around 2 lakh in 2024.
Due to Covid 19 infection, and use of life saving steroid intake, AVN as a side effect has surged significantly with estimated more than 5Lakh AVN patients.
- Avascular Necrosis. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537007/#:~:text=Also%20known%20as%20avascular%20necrosis,viability%20of%20the%20joint%20involved. Accessed on:6th April 2021.
- Steinberg DR, Steinberg ME. Osteonecrosis: an overview. Techniques in Orthopaedics. 2008 Mar 1;23(1):2-10.
- Baig SA, Baig MN. Osteonecrosis of the femoral head: etiology, investigations, and management. Cureus. 2018 Aug;10(8).
- Seamon J, Keller T, Saleh J, Cui Q. The pathogenesis of nontraumatic osteonecrosis. Arthritis. 2012;2012.
- Liu LH, Zhang QY, Sun W, Li ZR, Gao FQ. Corticosteroid-induced osteonecrosis of the femoral head: detection, diagnosis, and treatment in earlier stages. Chinese medical journal. 2017 Nov 5;130(21):2601.
- Dalal AA, Duh MS, Gozalo L, Robitaille MN, Albers F, Yancey S, Ortega H, Forshag M, Lin X, Lefebvre P. Dose-response relationship between long-term systemic corticosteroid use and related complications in patients with severe asthma. Journal of managed care & specialty pharmacy. 2016 Jul;22(7):833-47.